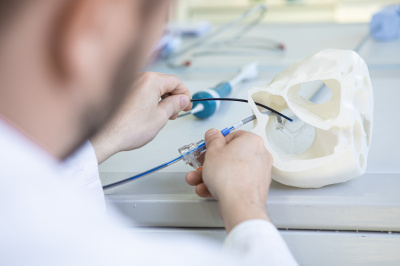
In cardiology, heart diseases are diagnosed and treated in a minimally invasive manner with the aid of catheters. The support offered by the biomaterial research carried out in Teltow allows cardiologists, for example, to now be able to print individual 3D models of patients' hearts so that they can plan and practice complex procedures down to the millimeter. Defective heart valves can be repaired with small clamp-shaped implants without having to replace the entire heart valve.
360° of science: Through the heart's labyrinth (The video is only available in german)
Note for the iOS operating system: For a free look around, please follow the link to our video on Youtube https://youtu.be/31t98Z_UNrI
The heart: a highly complex organ, whose beat determines our entire life. Medical procedures on the heart are increasingly being performed in a minimally invasively manner with catheters, which enables a more gentle treatment.
At the Institute for Active Polymers in Teltow, methods are being developed to provide cardiologists with the best possible support during complicated, minimally invasive medical procedures. A 3D printer can be used, for example, to create highly detailed models of a heart – personalized for individual patients on the basis of imaging diagnostics. These models allow cardiologists to plan and practice before the procedure, to ensure that their instruments reach the heart without any complications. In doing so, two catheters can also be used: One is equipped with a camera, the other is used to place an implant.
Defective heart valves can be repaired with small clamp-shaped implants without having to replace the entire heart valve.
Video: Interview with Markus Reinthaler (The video is only available in german. You can find the translation below in the transcription of the video)
Right to the Heart: Digital Images and 3D Printing
Minimally invasive heart valve procedures can be practiced on models that precisely match the organ’s individual anatomy.
By Lars Klaaßen
Illnesses afflicting the musculoskeletal and cardiovascular systems are the focus of clinical research at the Institute of Biomaterial Science. With a leaky heart valve, for example, open heart surgery was required up until a few years ago to replace the valve with an implant. For the elderly or for people with pre-existing conditions, this procedure was extremely challenging. It is now also possible to restore the natural valve using minimally invasive methods—theoretically.
In this type of treatment, a clip is inserted into the right atrium using a catheter. During the procedure, the edges of the leaky valve are connected by the clip at certain points. This at least reduces the leakage. As this is not a surgical procedure under visual control, good imaging is essential. Physicians have so far been using an ultrasound probe in order to view the area. The quality, however, is too often insufficient. “With the help of digital visualisation methods, a 3D printer and an ultrasound probe inserted directly into the heart cavity, we can remedy this problem,” says Markus Reinthaler. The director of “Structural Heart Disease” at the Charité’s Benjamin Franklin campus also works at the Hereon-Institute for Active Polymers, cooperating with other researchers towards finding this solution. The additional imaging option includes a small ultrasound probe (ICE catheter) inserted very close to the heart valve, improving the valve’s imaging. As cardiac structures differ greatly from patient to patient, methodical training is required to gain familiarity with each heart. Furthermore, two catheters are then in use: the probe and the implant-bearing catheter system.
“Our approach is an individual 3D heart model made of polymer, with which we can find and train the most suitable manoeuvre sequence for the probe with the corresponding positions and orientations,” says Reinthaler. For this purpose, three-dimensional heart models were created from the patients' CT data sets and a physical object was created using a 3D printer.
One study comparing patients treated with the previous and new procedure showed encouraging results: the use of the ICE probe with the 3D model training, made it possible to treat patients who could not have been treated using conventional imaging or could only have been treated to a limited extent.